 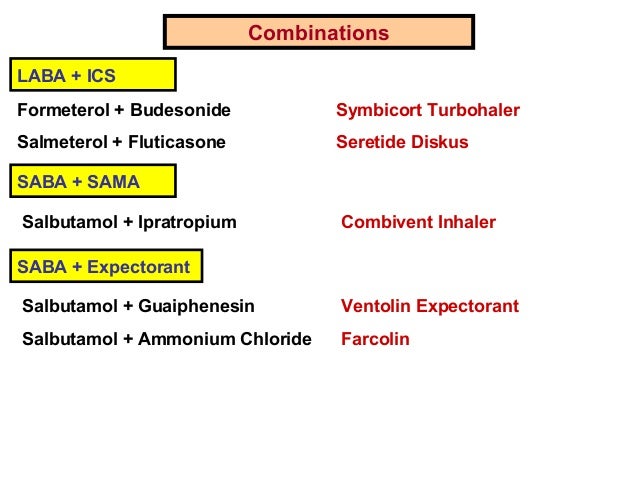
9, 10 Moreover, several of the emerging medications for COPD (both marketed and under development) utilize nebulizer technology. In addition, both patients and their caregivers are becoming increasingly satisfied with nebulized drug delivery and have reported benefits in symptom relief, ease of use, and improved quality of life when using this system. 2 Further, GOLD recommends evaluating the benefits of nebulizer treatment symptomatically and continuing treatment as long as similar benefits are not achievable by simpler, cheaper, and more portable alternatives. Although DPIs and pMDIs are the most commonly used devices 7, 8 and are recommended for long-term treatment in the vast majority of patients, 2 the Global Initiative for Chronic Obstructive Lung Disease (GOLD) strategy document recommends nebulizers for specific patient populations (eg, patients with very low inspiratory flow rates) in whom nebulizer treatment may provide more benefits than DPIs or MDIs. 1, 2 Four commonly prescribed inhalation devices, pressurized metered dose inhalers (pMDIs), dry powder inhalers (DPIs), slow mist inhalers (SMIs), and nebulizers, have similar efficacies in patients with COPD, 3 – 6 provided they are used appropriately. Inhaled pharmacologic therapy is a cornerstone of treatment for patients with COPD. This article reviews recent innovations in nebulized drug delivery and the important role of nebulized therapy in the treatment of COPD. As more drugs become available in solution formulations, patients with COPD and their caregivers are becoming increasingly satisfied with nebulized drug delivery, which provides benefits similar to drugs delivered by handheld inhalers in both symptom relief and improved quality of life. Dry powder inhalers and pressurized metered dose inhalers are the most commonly used drug delivery devices, but they may be inadequate in various clinical scenarios (eg, the elderly, the cognitively impaired, and hospitalized patients). Bronchodilators (β 2-agonists and antimuscarinics) are the mainstay of pharmacologic therapy in patients with COPD, with long-acting agents recommended for patients with moderate to severe symptoms or those who are at a higher risk for COPD exacerbations. 
There were no significant differences among the LAMAs and LAMA/LABAs within their respective classes.Īnticholinergics chronic obstructive pulmonary disease frequentist meta-analysis indirect treatment comparison mixed treatment comparison muscarinic antagonists.Current guidelines recommend inhaled pharmacologic therapy as the preferred route of administration for treating COPD. LAMA/LABA showed the greatest improvement in trough FEV 1 at weeks 12 and 24 compared with the other inhaled drug classes, while SAMA showed the least improvement. There were no significant differences in the incidences of adverse events among all treatment options. Similar trends were observed for the transition dyspnea index and St George's Respiratory Questionnaire outcomes. 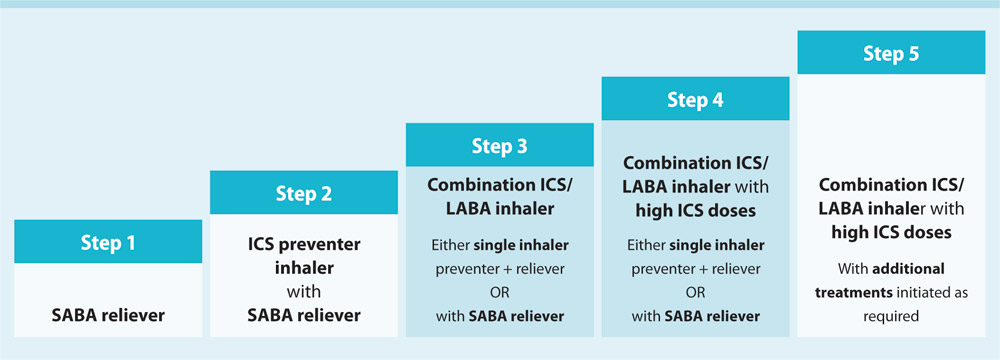
LAMA/LABAs had the highest probabilities of being ranked the best agents in FEV 1 improvement. Among the LAMAs, umeclidinium showed statistically significant improvement in trough FEV 1 at week 12 compared to tiotropium and glycopyrronium, but the results were not clinically significant. All LAMA/LABAs, except aclidinium/formoterol, were statistically significantly better than LAMA monotherapy and ICS/LABAs in improving trough FEV 1. LAMAs, LAMA/LABAs and ICS/LABAs led to a significantly greater improvement in trough FEV 1 compared with placebo and SAMA monotherapy at weeks 12 and 24. Inconsistency models were not statistically significant for all outcomes. 
A random-effects network meta-analysis combining direct and indirect evidence was conducted to examine the change from baseline in trough FEV 1, transition dyspnea index, St George's Respiratory Questionnaire and frequency of adverse events at weeks 12 and 24. We systematically reviewed 74 randomized controlled trials (74,832 participants) published up to 15 November 2017, which compared any of the interventions (SAMA, LAMA, LAMA/LABA and ICS/LABA ) with each other or with placebo. To assess the comparative efficacy of short-acting muscarinic antagonists (SAMAs), long-acting muscarinic antagonists (LAMAs), LAMA in combination with long-acting beta-agonists (LABAs LAMA/LABAs) and inhaled corticosteroids (ICS) in combination with LABA (ICS/LABAs) for the maintenance treatment of COPD. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
